Symptoms
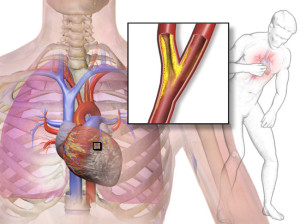
Angina is the word used to describe chest pain or chest discomfort due to poor blood supply to the heart. Not all chest pain is due to problems in the heart; problems in the lungs, chest wall, or stomach can all cause chest pain.
However, angina is the most worrisome cause of chest pain and as such all patients presenting with chest pain should be evaluated by a doctor to decide whether the pain is in fact coming from the heart.
Typical symptoms suggesting that the pain is related to the heart is a central discomfort in the chest, often described as a tightness or heaviness. This may radiate (move) to the neck, jaw, or left arm.
Usually, the pain is brought on by physical or emotional stress but may occur at rest. However, many patients do not get ‘typical’ symptoms.
Pain that is thought to be angina and that occurs at rest, awakens an individual at night, or lasts more than 15 minutes suggests an emergency, and patients should call an ambulance.
Chest pain is investigated by a full and detailed history and examination by your cardiologist, an ECG and usually an Exercise Treadmill Test.
If abnormalities are found the next step is usually a coronary angiogram.
Breathlessness may be a sign of heart failure. Additional symptoms to suggest this are problems with breathing when lying flat and swelling of the ankles.
Occasionally breathlessness may be a form of ‘angina’. In this case rather than chest pain patients develop breathlessness on exertion due to poor blood supply to the heart.
Breathlessness may of course be related to the lungs when more commonly there will be symptoms of coughing or wheezing.
Palpitations are common. These can be experienced as an awareness of the odd extra beat particularly made worse with caffeine or alcohol. These are likely to be ‘extra systoles’.
Palpitations may also be an awareness of fast and/or heavy heartbeats, which may represent an arrhythmia or tachycardia such as an SVT (supraventricular tachycardia), atrial fibrillation or ventricular tachycardia.
Patients should discuss any extra hearts beats or palpitations with their doctor. If palpitations last more than seconds, are associated with symptoms of dizziness, sweating or chest pain or if there is a family history of heart disease they should be seen for a full cardiac check up.

All patients suffering with sustained palpitations and fainting need to be seen on an urgent basis.
Investigations will normally include an ECG, Echo scan and 24 hour heart monitor.


All blackouts need to be investigated. Simple causes of blackouts may be vasovagal syncope when certain triggers such as fright, pain, prolonged standing, urinating or even coughing, may cause the blood pressure and/or heart rate to fall.
Commonly there are warning signs of sweating, nausea or dizziness prior to collapse. Once investigated and reassured the treatments are simple and the condition benign.
Worrisome collapses are those with no prior warning, those associated with any other symptoms such as chest pain or palpitations.
Anyone collapsing on exercise, especially at a young age (below 35 years of age) and those in whom there is a family history of premature cardiac disease or sudden death need to see a cardiologist with an interest in inherited cardiac disease.
Investigations will normally include an ECG, Echo scan and 24 hour heart monitor.



